Young Adults With Type 2 Diabetes: A Journey Begins: Taking the Long View
Cardiology
Medscape
News & Perspective
Your one-stop resource for medical news, clinical reference, and education.
Sign up for FREEAlready a member? Log in
UK News & Perspectives View All
Featured Cardiology News & Perspectives
Latest News View All
-
 ACC 2024Telemedicine Boosts GDMT Rates for HFrEF in Navajo Nation
ACC 2024Telemedicine Boosts GDMT Rates for HFrEF in Navajo Nation -
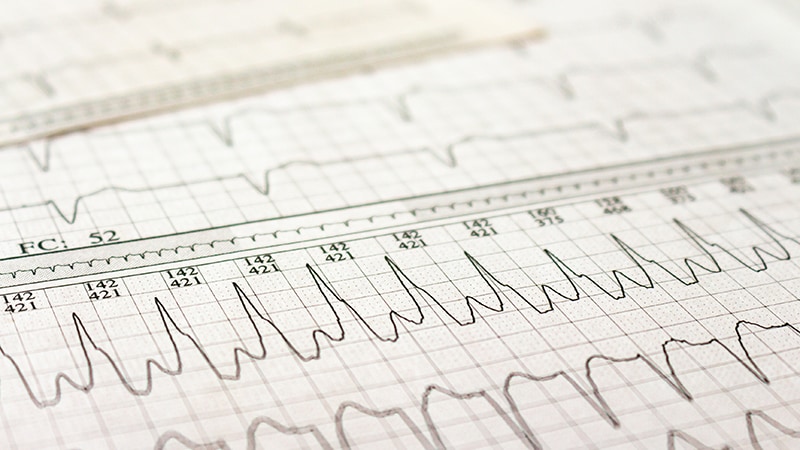 Heart Failure, Not Stroke, Most Common Complication of A-Fib
Heart Failure, Not Stroke, Most Common Complication of A-Fib -
 Antipsychotics for Dementia Pose Wide-Ranging Health Risks
Antipsychotics for Dementia Pose Wide-Ranging Health Risks -
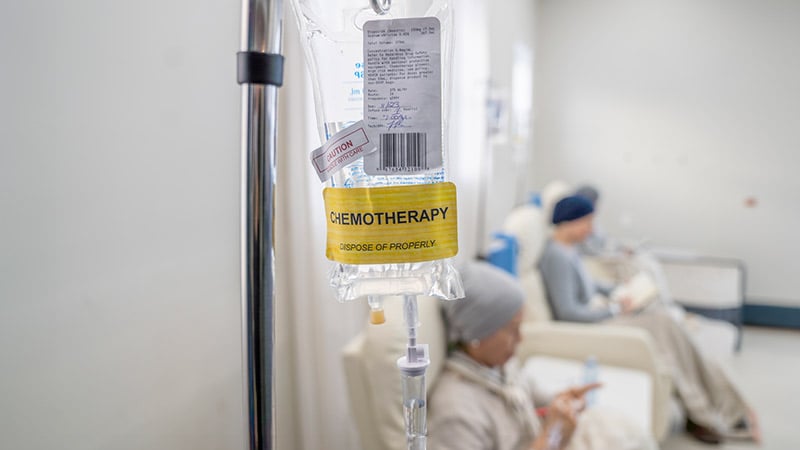 ACC 2024Adding ACEI to Chemotherapy Does Not Prevent Cardiotoxicity
ACC 2024Adding ACEI to Chemotherapy Does Not Prevent Cardiotoxicity -
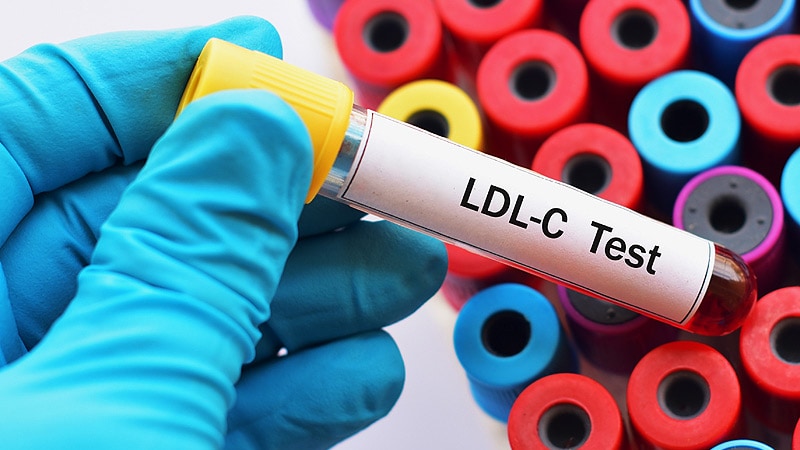 ACC 2024Novel PCSK9 Inhibitor Reduced LDL by 50%
ACC 2024Novel PCSK9 Inhibitor Reduced LDL by 50% -
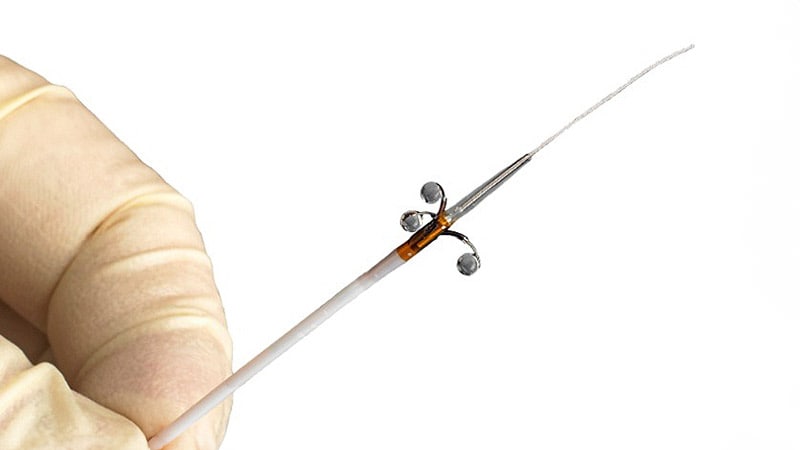 ACC 2024Alcohol-Mediated Renal Denervation Promising in Hypertension
ACC 2024Alcohol-Mediated Renal Denervation Promising in Hypertension -
 Pregnancy Complications Increase Risk for Early Death
Pregnancy Complications Increase Risk for Early Death -
 ACC 2024Exercise Plus Protein Boosts TAVR Outcomes in Frail Patients
ACC 2024Exercise Plus Protein Boosts TAVR Outcomes in Frail Patients
Trending With Cardiologists
Perspectives View All
Columnists
mtv
Journal Articles View All
-
What Is a Normal Left Ventricular Ejection Fraction?
-
CV Outcomes After COVID-19 Vaccine-Associated Myocarditis
-
Exercise-Induced Chest Pain: Ischemia or Something Else
-
Sex Differences in Poststroke Cognitive Impairment
-
Lessons in CVD Prevention From Jackie Robinson
-
Established and Emerging Lipid-Lowering Drugs for CVD Prevention
Medscape Essentials
Cases & Quizzes View All
Conferences View All
View AllBusiness of Medicine View All
Medscape Editorial Collaborations
Advisory Board
Senior Editorial Director
EXECUTIVE EDITOR
Chief Cardiology Correspondent